Health A-Z

Osteoporosis
Overview
- Osteoporosis is a generalised bone disease characterised by diminished bone mineral density and bone mass with an increased risk of fractures (broken bones)¹.
- Osteoporosis is a “silent” disease as there are typically no symptoms until a bone is broken².
- Fractures can occur in any bones but happen most often in bones of the hip, vertebrae in the spine, and wrist².
- It has been estimated that more than 200 million people are suffering from osteoporosis worldwide, with increasing prevalence³.
- 1 in 3 women and 1 in 5 men, over the age of 50 years, will experience osteoporosis fractures in their lifetime³.
Symptoms and Signs

Back pain, caused by a fractured or collapsed vertebrae

Loss of height over time (more than 2 inches)

Curved and stooped shape to the spine

Bone that breaks much easier than expected

Signs and Symptoms

Back pain, caused by a fractured or collapsed vertebrae

Loss of height over time (more than 2 inches)

Curved and stooped shape to the spine

Bone that breaks much easier than expected
Causes and risk factors
- Age The older you are, the more likely you are to have osteoporosis. Around 75% of fractures due to osteoporosis happen in people aged 65 and over⁵.
- Gender Women are more likely to develop osteoporosis than men⁵.
- Family history⁵
- Bone structure and body weight⁵
- Menopause/ hysterectomy Oestrogen has a protective effect on bone, and with menopause women start to lose bone at a faster rate. Therefore, women who have early menopause (before age 45) or have had a hysterectomy, are at greater risk⁵.
- Long term use of medication⁵
- Other diseases Some diseases such as rheumatoid arthritis, thyroid disease, chronic liver and kidney disease place people at a higher risk of osteoporosis⁵.
- Inadequate amounts of dietary calcium⁵
- Low vitamin D levels⁵
- Lack of physical activity⁵
- Cigarette smoking⁵
- Alcohol intake⁵ Drinking more than two standard drinks per day increases the risk of fracture.
- Caffeine intake⁵ Drinking more than three cups of coffee or equivalent per day increases the risk of fracture.
- Frequent falls⁵ People who have a tendency to fall are at higher risk of fracture.
Causes and risk factors
- Age The older you are, the more likely you are to have osteoporosis. Around 75% of fractures due to osteoporosis happen in people aged 65 and over⁵.
- Gender Women are more likely to develop osteoporosis than men⁵.
- Family history⁵
- Bone structure and body weight⁵
- Menopause/ hysterectomy Oestrogen has a protective effect on bone, and with menopause women start to lose bone at a faster rate. Therefore, women who have early menopause (before age 45) or have had a hysterectomy, are at greater risk⁵.
- Long term use of medication⁵
- Other diseases Some diseases such as rheumatoid arthritis, thyroid disease, chronic liver and kidney disease place people at a higher risk of osteoporosis⁵.
- Inadequate amounts of dietary calcium⁵
- Low vitamin D levels⁵
- Lack of physical activity⁵
- Cigarette smoking⁵
- Alcohol intake⁵ Drinking more than two standard drinks per day increases the risk of fracture.
- Caffeine intake⁵ Drinking more than three cups of coffee or equivalent per day increases the risk of fracture.
- Frequent falls⁵ People who have a tendency to fall are at higher risk of fracture.
Supplement recommendations
Calcium
Benefits
Bone health
Nerve conduction
Muscle contraction
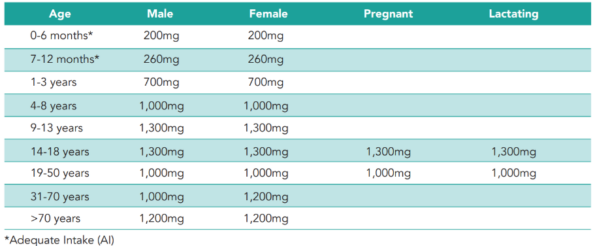
Recommended dosage
Recommended Dietary Allowances (RDAs) for calcium⁷
Vitamin D
Benefits
Bone health
Numerous research showed that adequate intake of vitamin D helps to ease the risk of rickets and osteomalacia. A daily intake of 5,000–10,000 IU of vitamin D is recommended for children age 1 year or older who suffer from vitamin D deficiency rickets and the dose can be reduced to 400IU daily when there is radiographic evidence of healing⁸. The mechanism of vitamin D promotes bone mineralisation included improving intestinal absorption of calcium and phosphorus as well as facilitating osteoclast function⁹.
Immunity system
Vitamin D receptors are found in immune system agents such as B cells, T cells, and antigen-presenting cells¹⁰. It enhances the differentiation of macrophages which helps to boost immunity toward bacterial and viral agents. Furthermore, vitamin D helps to prevent respiratory tract infections via the induction of antimicrobial peptides that build protection against respiratory pathogens¹¹. Research indicates that a therapeutic dose of vitamin D (200IU/day) resulted in a significant decrease (42%) in the incidence of influenza infection among school children¹².
Cognitive function
A meta-analysis reported that the elderly with vitamin D insufficiency may increase the risk of incident cognitive impairment, semantic memory, and executive function decline which correlated with an increased risk of Alzheimer’s disease. Indeed, vitamin D helps to prevent cognitive decline by decreasing β-amyloid synthesis and thereby protecting neurodegeneration induced by inflammation¹³.
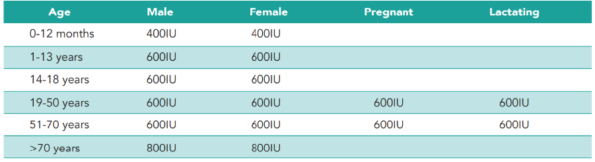
Recommended dosage
Recommended Dietary Allowances (RDAs) for vitamin D¹⁸:
Vitamin K2
Benefits
Arterial calcification
Vitamin K2 activates matrix GLA protein (MGP), a calcification inhibitor that suppresses the accumulation of calcium on the vessel wall. This helps to prevent cardiovascular disease caused by the thickening of vessel wall via calcified plaques. Research indicates that death caused by cardiovascular issues related to arterial calcification reduce 50% after daily intake of at least 32mg Vitamin K2 among people over 55 years¹⁹,²⁰.
Osteoporosis
Vitamin K2 plays an important role in promoting bone mineralisation by activating osteocalcin synthesis by osteoblast. Activated osteocalcin will bind calcium into the bone matrix which improves skeleton strength and less susceptible to fracture²¹. Besides, vitamin K2 also protects osteoblasts from apoptosis which leads to reduction in cortical porosity²². Studies indicate that daily intake of 1.5mg short-chain menaquinone-4 (MK-4) can improve vertebral bone mineral density in postmenopausal women with osteoporosis²³.
Brain disorder
Vitamin K2 involves in brain development by activating growth arrest-specific gene 6 (Gas6) and protein S which works on chemotaxis, mitogenesis, and cell growth. Sphingolipids synthesis by vitamin K2 is important in the proliferation, differentiation, and survival of brain cells. Vitamin K2 can protect neural cells from neurotoxic-amyloid which have the potential to cause Alzheimer’s disease²⁴.
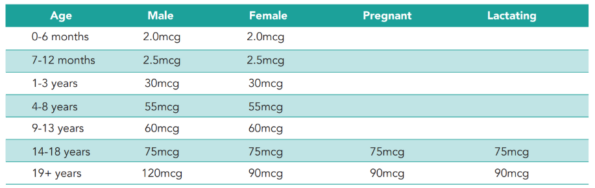
Recommended dosage
Recommended Dietary Allowances (RDAs) for vitamin K²⁵
Supplement recommendations 1
Calcium
Benefits
Bone health
Nerve conduction
Muscle contraction
Recommended dosage
Recommended Dietary Allowances (RDAs) for calcium⁷

Supplement recommendations 2
Calcium
Benefits
Bone health
Nerve conduction
Muscle contraction
Recommended dosage
Recommended Dietary Allowances (RDAs) for calcium⁷

Supplement recommendations
Vitamin D
Benefits
Bone health
Numerous research showed that adequate intake of vitamin D helps to ease the risk of rickets and osteomalacia. A daily intake of 5,000–10,000 IU of vitamin D is recommended for children age 1 year or older who suffer from vitamin D deficiency rickets and the dose can be reduced to 400IU daily when there is radiographic evidence of healing⁸. The mechanism of vitamin D promotes bone mineralisation included improving intestinal absorption of calcium and phosphorus as well as facilitating osteoclast function⁹.
Immunity system
Vitamin D receptors are found in immune system agents such as B cells, T cells, and antigen-presenting cells¹⁰. It enhances the differentiation of macrophages which helps to boost immunity toward bacterial and viral agents. Furthermore, vitamin D helps to prevent respiratory tract infections via the induction of antimicrobial peptides that build protection against respiratory pathogens¹¹. Research indicates that a therapeutic dose of vitamin D (200IU/day) resulted in a significant decrease (42%) in the incidence of influenza infection among school children¹².
Cognitive function
A meta-analysis reported that the elderly with vitamin D insufficiency may increase the risk of incident cognitive impairment, semantic memory, and executive function decline which correlated with an increased risk of Alzheimer’s disease. Indeed, vitamin D helps to prevent cognitive decline by decreasing β-amyloid synthesis and thereby protecting neurodegeneration induced by inflammation¹³.
Recommended dosage
Recommended Dietary Allowances (RDAs) for vitamin D¹⁸:

Supplement recommendations
Vitamin K2
Benefits
Arterial calcification
Vitamin K2 activates matrix GLA protein (MGP), a calcification inhibitor that suppresses the accumulation of calcium on the vessel wall. This helps to prevent cardiovascular disease caused by the thickening of vessel wall via calcified plaques. Research indicates that death caused by cardiovascular issues related to arterial calcification reduce 50% after daily intake of at least 32mg Vitamin K2 among people over 55 years¹⁹,²⁰.
Osteoporosis
Vitamin K2 plays an important role in promoting bone mineralisation by activating osteocalcin synthesis by osteoblast. Activated osteocalcin will bind calcium into the bone matrix which improves skeleton strength and less susceptible to fracture²¹. Besides, vitamin K2 also protects osteoblasts from apoptosis which leads to reduction in cortical porosity²². Studies indicate that daily intake of 1.5mg short-chain menaquinone-4 (MK-4) can improve vertebral bone mineral density in postmenopausal women with osteoporosis²³.
Brain disorder
Vitamin K2 involves in brain development by activating growth arrest-specific gene 6 (Gas6) and protein S which works on chemotaxis, mitogenesis, and cell growth. Sphingolipids synthesis by vitamin K2 is important in the proliferation, differentiation, and survival of brain cells. Vitamin K2 can protect neural cells from neurotoxic-amyloid which have the potential to cause Alzheimer’s disease²⁴.
Recommended dosage
Recommended Dietary Allowances (RDAs) for vitamin K²⁵

Diet & lifestyle recommendations
- Get more calcium from food or supplement.
- Get sufficient vitamin D which helps body to absorb calcium.
- Eat a balanced and healthy diet.
- Take calcium-enriched food and avoid diet high in protein and/or sodium which can increase calcium loss²⁶.
- Exercise regularly.
- Do regular weight-bearing and strength-training activities.
- Avoid both cigarette smoking and excessive alcohol consumption as both have been proven to accelerate bone loss⁵.
References :
- Maria Becheva, D. T. (2020). Prevention and treatment of osteoporosis. Pharmacia 67(4), 81–185.
- Health, N. I. (n.d.). National Institutes of Health. Retrieved from Osteoporosis Overview: https://www.bones.nih.gov/health-info/bone/osteoporosis/overview
- Tümay Sözen, Lale Özışık, Nursel Çalık Başaran. (2017). An overview and management of osteoporosis. Eur J Rheumatol, 46-56.
- Mayo Foundation for Medical Education and Research. (2022). Osteoporosis. Retrieved from Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/osteoporosis/symptoms-causes/syc-20351968
- International Osteoporosis Foundation. (2022). About Osteoporosis. Retrieved from International Osteoporosis Foundation: https://www.osteoporosis.foundation/patients/about-osteoporosis
- Calcium. (2020). Retrieved from https://www.hsph.harvard.edu/nutritionsource/calcium/#:~:text=Calcium%20is%20a%20mineral%20most,heart%20rhythms%20and%20nerve%20functions
- Calcium. Fact sheet for health professional. Retrieved from https://ods.od.nih.gov/factsheets/Calcium HealthProfessional/#:~:text=Average%20daily%20intakes%20of%20calcium,to%201%2C015%20mg%20% B18%5D
- Sahay, M., & Sahay, R. (2012). Rickets-vitamin D deficiency and dependency. Indian journal of endocrinology and metabolism, 16(2), 164–176. https://doi.org/10.4103/2230-8210.93732
- Li, R.N., Yu, T.W.,Chih, L.K., Kuo, H.C. (2014). Calcium and Vitamin D Supplementation on Bone Health: Current Evidence and Recommendations. International Journal of Gerontology, 8(14): 183-188. https://doi.org/10.1016/j.ijge.2014.06.001
- Pludowski, P., Holick, M. F., Pilz, S. et al. (2013). Vitamin D effects on musculoskeletal health, immunity, autoimmunity, cardiovascular disease, cancer, fertility, pregnancy, dementia and mortality—A review of recent evidence. Autoimmunity Reviews, 12: 976-989. http://dx.doi.org/10.1016/j.autrev.2013.02.004
- Martineau, A.R., Jolliffe, D.A., Hooper, R.L., et al. (2017). Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ, 356:i6583. https://doi.org/10.1136/bmj.i6583
- Urashima, M., Segawa, T., Okazaki, M., Kurihara, M., Wada, Y., & Ida, H. (2010). Randomized trial of vitamin D supplementation to prevent seasonal influenza A in schoolchildren. The American journal of clinical nutrition, 91(5), 1255–1260. https://doi.org/10.3945/ajcn.2009.29094
- Liu, W., Zhou, C., Wang, Y.S., et al. (2021). Vitamin D Deficiency Is Associated with Disrupted Cholesterol Homeostasis in Patients with Mild Cognitive Impairment. The Journal of Nutrition, 151(12): 3865-3873. https://doi.org/10.1093/jn/nxab296
- Danik, J. S., & Manson, J. E. (2012). Vitamin D and cardiovascular disease. Current treatment options in cardiovascular medicine, 14(4), 414–424. https://doi.org/10.1007/s11936-012-0183-8
- Giovannucci, E., Liu, Y., Hollis, B. W., & Rimm, E. B. (2008). 25-hydroxyvitamin D and risk of myocardial infarction in men: a prospective study. Archives of internal medicine, 168(11), 1174–1180. https://doi.org/10.1001/archinte.168.11.1174
- Pilz, S., Verheyen, N., Grubler, M. R. et al. (2016). Vitamin D and cardiovascular disease Prevention. Nature Review Cardiology, 13: 404–417. http://dx.doi.org/10.1038/nrcardio.2016.73
- Pittas A.G., Dawson-Hughes B., Li T., Van Dam R.M., et al. (2006). Vitamin D and calcium intake in relation to type 2 diabetes in women. Diabetes Care 29, 650–656. http://dx.doi.org/10.2337/diacare.29.03.06.dc05-1961.
- Institute of Medicine, Food and Nutrition Board. (2010). Dietary Reference Intakes for Calcium and Vitamin D. National Academy Press. DC, Washington.
- 1Maresz K. (2015). Proper Calcium Use: Vitamin K2 as a Promoter of Bone and Cardiovascular Health. Integrative medicine (Encinitas), 14(1), 34–39. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4566462/
- Geleijnse, J.M., Vermeer, C. & Grobbee, D. E., et al. (2004). Dietary intake of menaquinone is associated with a reduced risk of coronary heart disease: the Rotterdam Study. J Nutr.134(11):3100–3105.
- Jacob, A. (2013). Vitamin K2 — A Little-Known Nutrient Can Make a Big Difference in Heart and Bone Health. Retrieved from: https://www.todaysdietitian.com/newarchives/060113p54.shtml
- 3. Mynei, V.D. & Mezey, E. (2016). Regulation of bone remodelling by vitamin K2. Oral Diseases, 23(8), 1021-1028. https://doi.org/10.1111/odi.12624 https://onlinelibrary.wiley.com/doi/full/10.1111/odi.12624
- 4. Huang, Z. B., Wan, S. L., Lu, Y. J., Ning, L., Liu, C., & Fan, S. W. (2015). Does vitamin K2 play a role in the prevention and treatment of osteoporosis for postmenopausal women: a meta-analysis of randomized controlled trials. Osteoporosis International, 26(3), 1175–1186. https://doi.org/10.1007/s00198-014-2989-6
- Vos, M., Esposito, G., Edirisinghe, J. N., Vilain, S., Haddad, D. M. & Slabbaert, J. R., et al. (2012). Vitamin K2 is a mitochondrial electron carrier that rescues pink1 deficiency. Science, 336(6086), 1306–1310. https://doi.org/10.1126/science.1218632 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8483258/#ref15
- Institute of Medicine. (2001). Dietary reference intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. National Academy Press. DC, Washington. https://ods.od.nih.gov/factsheets/vitamink-healthprofessional/#h2
- HealthHub. (n.d.). Daily Calcium Intake – For Greater Bone Strength. Retrieved from HealthHub: https://www.healthhub.sg/live-healthy/518/Calcium%20-%20For%20Greater%20Bone%20Strength
You might also be interested in
Osteoarthritis
- Osteoarthritis (OA) is the most common type of arthritis which affects 10% of the global population1¹.
- In global, it is one of the most frequent causes of pain or aching, stiffness, decreased flexibility and swelling in adults². It commonly affects people over 60 years of age.
- OA is caused by wear and tear due to excessive use over the years or to old injuries in the affected joints³.
- Osteoarthritis mostly affects the large weight-bearing joints like the knees, hips and spine, causing pain and stiffness which are worst at the end of the day. The affected person may have difficulty in walking, climbing stairs, squatting or kneeling⁴.
Insomnia
- Insomnia is a prevalent sleep disorder that can profoundly impact a person’s health and wellbeing.
- Various studies worldwide have shown that the prevalence of insomnia is approximately 10-30% of the population, some even as high as 50%-60%¹.
- Insomnia is common in older adults, females and people with medical and mental ill health¹.
- Insomnia has been associated with a wide range of deleterious health consequences, including an increased risk of hypertension, cardiovascular disease, diabetes, anxiety and depression².
Gastroesophageal reflux disease (GERD)
- Gastroesophageal reflux disease (GERD) is a digestive disorder that occurs when acidic stomach juices, or food and fluids back up from the stomach into the esophagus¹.
- The prevalence of GERD in Asia is low, ranging from 2.5% to 7.1% for weekly reflux, 3.8% to 4.6% for twice weekly reflux, and 2.1% for daily reflux, but it might be due to low awareness of the disorder².
- The prevalence of symptom-based GERD in Southeast Asia has been rising3 and was estimated to be 6.3%–18.3% from 2005–2010⁴.
- Left untreated, GERD can result in an esophageal mucosal injury known as reflux esophagitis where persistent backflow of acidic digestive juices will damage the lining of the oesophagus over time⁵.
Brain Fog
- Brain fog is used to describe ‘a usually tempporary state of diminished mental capacity marked by inability to concentrate or to think or reason clearly.¹
- Brain fog is not a formal diagnosis or medical condition but a series of neuropsychologic symptoms related to mild cognitive impairment which may affect daily function.
- Although there are no statistics on the prevalence of brain fog specifically, it was estimated that around 600 million people worldwide suffer from cognitive dysfunction.²
- It has been reported that brain fog is one of the most common long COVID symptoms among survivors.³
Constipation
- Constipation is a common functional gastrointestinal disorder, with prevalence in the general population of approximately 20%. It is more prevalent in females and the elderly¹.
- Constipation is both a symptom and, when chronic, a multisymptomatic disorder, and it can overlap with other gastrointestinal tract disorders such as dyspepsia and gastroesophageal reflux disease².
- Constipation most commonly refers to infrequent bowel movements. It is defined as having a bowel movement less than 3 times per week³.
- Chronic constipation is difficult and/or rare passage of stools that lasts for several months that can interfere people’s ability to go about their daily activities. It may also cause people to strain excessively to have bowel movement⁴.







