
Health A-Z

Gastroesophageal reflux disease (GERD)
Overview
- Gastroesophageal reflux disease (GERD) is a digestive disorder that occurs when acidic stomach juices, or food and fluids back up from the stomach into the esophagus¹.
- The prevalence of GERD in Asia is low, ranging from 2.5% to 7.1% for weekly reflux, 3.8% to 4.6% for twice weekly reflux, and 2.1% for daily reflux, but it might be due to low awareness of the disorder².
- The prevalence of symptom-based GERD in Southeast Asia has been rising3 and was estimated to be 6.3%–18.3% from 2005–2010⁴.
- Left untreated, GERD can result in an esophageal mucosal injury known as reflux esophagitis where persistent backflow of acidic digestive juices will damage the lining of the oesophagus over time⁵.
Symptoms and Signs

Heartburn⁶

Regurgitation⁶

Vomiting⁶

Difficulty swallowing⁶

Burning feeling in stomach or near chest area⁷

Chest pain⁷

Indigestion⁷

Signs and Symptoms

Heartburn⁶

Regurgitation⁶

Vomiting⁶

Difficulty swallowing⁶

Burning feeling in stomach or near chest area⁷

Chest pain⁷

Indigestion⁷
Causes and risk factors
- Obesity⁸
- Hiatal hernia, a condition where the upper part of the stomach moves up into the chest through an opening in the diaphragm, which lowers the pressure in the oesophageal sphincter⁸
- Stress⁹
- Certain foods and beverages, such as spicy or fatty foods, chocolate, peppermint, coffee, or alcoholic beverages¹⁰
- Smoking¹¹
- Use of certain medications, including calcium channel blockers, painkillers, sedatives, and antidepressants¹²
Causes and risk factors
- Obesity⁸
- Hiatal hernia, a condition where the upper part of the stomach moves up into the chest through an opening in the diaphragm, which lowers the pressure in the oesophageal sphincter⁸
- Stress⁹
- Certain foods and beverages, such as spicy or fatty foods, chocolate, peppermint, coffee, or alcoholic beverages¹⁰
- Smoking¹¹
- Use of certain medications, including calcium channel blockers, painkillers, sedatives, and antidepressants¹²
Supplement recommendations
Fermented soy peptide
Benefits
Symptoms of GERD
It has been shown that fermented soy improved some indicators of heartburn-related quality of life and may have potential benefits for reducing heartburn frequency over time¹³.
Studies on gastritis patients have shown that taking a patented food supplement based on non-GMO fermented soy, Gastro-AD® 30 minutes before a meal for 30 days helps in rapid and long-lasting relief within 15 minutes or less1¹⁴,¹⁵. Gastro-AD® not only consisted of fermented soy peptides but also a significant proportion of heat-inactivated Rosell-187 (R0187) strain of lactic acid bacteria. It is shown that R0187 may have a suppressive effect on interleukin⁸, the inflammatory cytokine, in intestinal cells¹⁶. This may help with modulating the inflammation response in the mucosal microenvironment and preventing stomach ulcers.
Recommended dosage
Soy protein is most used in daily doses of up to 40-60 grams for 4 months up to 6 months. Gastro-AD® has been tested in several clinical studies, on approximately 600 subjects. It was shown to be tolerable for Gastro-AD® up to 15g per day for 30 days¹⁴. Results show that it provides quick relief from ulcer symptoms including heartburn, pain, vomiting and constipation.
Symptoms of GERD
2g to 5g of Gastro-AD®, 3 times daily, 30 minutes before meals for 30 days14,15.
Licorice root extract
Mechanism of action
It exerts anti-H. pylori activity by inhibiting protein synthesis, DNA Gyrase, and dihydrofolate reductase¹⁷. It also interrupts the inflammatory cascade¹⁸ and possesses antioxidant properties¹⁹.
Benefits
Indigestion
Among various gastrointestinal disorders, functional dyspepsia also known as indigestion is one of the most common clinical conditions among the general population. The general symptoms include upper abdominal fullness, epigastric pain, belching, bloating, early satiety, nausea, vomiting, regurgitation, heartburn, and loss of appetite. Oral licorice might improve symptoms of dyspepsia when used in combination with other ingredients.
Meanwhile, a randomised, double-blind, placebo-controlled study showed that deglycyrrhizinated licorice, DGL (GutGard®) helps relieve occasional indigestion²⁰. In the study, the subjects received a specified dose of GutGard® for 15 and 30 days, and the severity of the complaint and quality of life significantly improved compared to the placebo group.
Recommended dosage
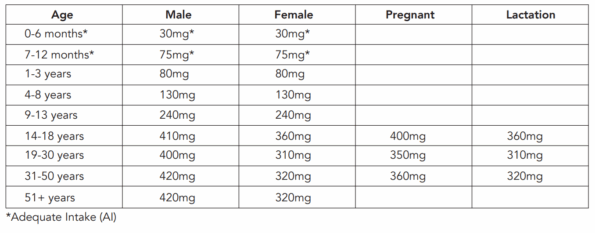
Recommended dietary allowances (RDAs) for magnesium¹⁷
Konjac
Mechanism of action
Like other forms of dietary fiber, konjac glucomannan is considered a “bulk-forming laxative.” Glucomannan promotes a larger, bulkier stool that passes through the colon more easily, requiring less pressure and subsequently less straining to expel¹⁸.
Benefits
Constipation
Studies shown that glucomannan may provide relief in constipation through the improvement of probiotic bacteria counts in faeces (colonicecology) after daily supplementation of 1.5g of konjac glucomannan for 21 days. Bowel movement function was increased by 30%¹⁹. The mean defecation frequency and dry faecal mass increased due to the presence of plant and soluble materials from supplementation of konjac glucomannan²⁰.
Inflammatory bowel disease (IBD)
Daily consumption of konjac glucomannan hydrolysates was shown to enhance capacity to bind pathogens and prevent this from binding the gut’s lining, stimulating topical healing, regulating immunity and ability to form systemic immune responses among healthy people with IBD and associated gut conditions. It is function as soluble dietary fibre as well as prebiotic²¹.
Recommended dosage²²
Konjac is normally added to foods as a thickening agent and dietary fiber source. Typical doses used as treatment by adults is ranging from 3g to 4g daily for up to 3 months.
Supplement recommendations 1
Fermented soy peptide
Benefits
Symptoms of GERD
It has been shown that fermented soy improved some indicators of heartburn-related quality of life and may have potential benefits for reducing heartburn frequency over time¹³.
Studies on gastritis patients have shown that taking a patented food supplement based on non-GMO fermented soy, Gastro-AD® 30 minutes before a meal for 30 days helps in rapid and long-lasting relief within 15 minutes or less1¹⁴,¹⁵. Gastro-AD® not only consisted of fermented soy peptides but also a significant proportion of heat-inactivated Rosell-187 (R0187) strain of lactic acid bacteria. It is shown that R0187 may have a suppressive effect on interleukin⁸, the inflammatory cytokine, in intestinal cells¹⁶. This may help with modulating the inflammation response in the mucosal microenvironment and preventing stomach ulcers.
Recommended dosage
Soy protein is most used in daily doses of up to 40-60 grams for 4 months up to 6 months. Gastro-AD® has been tested in several clinical studies, on approximately 600 subjects. It was shown to be tolerable for Gastro-AD® up to 15g per day for 30 days¹⁴. Results show that it provides quick relief from ulcer symptoms including heartburn, pain, vomiting and constipation.
Symptoms of GERD
2g to 5g of Gastro-AD®, 3 times daily, 30 minutes before meals for 30 days14,15.
Supplement recommendations 2
Fermented soy peptide
Benefits
Symptoms of GERD
It has been shown that fermented soy improved some indicators of heartburn-related quality of life and may have potential benefits for reducing heartburn frequency over time¹³.
Studies on gastritis patients have shown that taking a patented food supplement based on non-GMO fermented soy, Gastro-AD® 30 minutes before a meal for 30 days helps in rapid and long-lasting relief within 15 minutes or less1¹⁴,¹⁵. Gastro-AD® not only consisted of fermented soy peptides but also a significant proportion of heat-inactivated Rosell-187 (R0187) strain of lactic acid bacteria. It is shown that R0187 may have a suppressive effect on interleukin⁸, the inflammatory cytokine, in intestinal cells¹⁶. This may help with modulating the inflammation response in the mucosal microenvironment and preventing stomach ulcers.
Recommended dosage
Soy protein is most used in daily doses of up to 40-60 grams for 4 months up to 6 months. Gastro-AD® has been tested in several clinical studies, on approximately 600 subjects. It was shown to be tolerable for Gastro-AD® up to 15g per day for 30 days¹⁴. Results show that it provides quick relief from ulcer symptoms including heartburn, pain, vomiting and constipation.
Symptoms of GERD
2g to 5g of Gastro-AD®, 3 times daily, 30 minutes before meals for 30 days14,15.
Supplement recommendations
Licorice root extract
Mechanism of action
It exerts anti-H. pylori activity by inhibiting protein synthesis, DNA Gyrase, and dihydrofolate reductase¹⁷. It also interrupts the inflammatory cascade¹⁸ and possesses antioxidant properties¹⁹.
Benefits
Indigestion
Among various gastrointestinal disorders, functional dyspepsia also known as indigestion is one of the most common clinical conditions among the general population. The general symptoms include upper abdominal fullness, epigastric pain, belching, bloating, early satiety, nausea, vomiting, regurgitation, heartburn, and loss of appetite. Oral licorice might improve symptoms of dyspepsia when used in combination with other ingredients.
Meanwhile, a randomised, double-blind, placebo-controlled study showed that deglycyrrhizinated licorice, DGL (GutGard®) helps relieve occasional indigestion²⁰. In the study, the subjects received a specified dose of GutGard® for 15 and 30 days, and the severity of the complaint and quality of life significantly improved compared to the placebo group.
Recommended dosage
Recommended dietary allowances (RDAs) for magnesium¹⁷

Supplement recommendations
Konjac
Mechanism of action
Like other forms of dietary fiber, konjac glucomannan is considered a “bulk-forming laxative.” Glucomannan promotes a larger, bulkier stool that passes through the colon more easily, requiring less pressure and subsequently less straining to expel¹⁸.
Benefits
Constipation
Studies shown that glucomannan may provide relief in constipation through the improvement of probiotic bacteria counts in faeces (colonicecology) after daily supplementation of 1.5g of konjac glucomannan for 21 days. Bowel movement function was increased by 30%¹⁹. The mean defecation frequency and dry faecal mass increased due to the presence of plant and soluble materials from supplementation of konjac glucomannan²⁰.
Inflammatory bowel disease (IBD)
Daily consumption of konjac glucomannan hydrolysates was shown to enhance capacity to bind pathogens and prevent this from binding the gut’s lining, stimulating topical healing, regulating immunity and ability to form systemic immune responses among healthy people with IBD and associated gut conditions. It is function as soluble dietary fibre as well as prebiotic²¹.
Recommended dosage²²
Konjac is normally added to foods as a thickening agent and dietary fiber source. Typical doses used as treatment by adults is ranging from 3g to 4g daily for up to 3 months.
Diet & lifestyle recommendations
- Maintain a healthy weight
- Have meals at least 2 to 3 hours before lying down³¹
- Eat smaller portion for each mealtime, avoid overeating³¹
- Avoid food and beverages that may trigger heartburn, such as fatty meals, citrus fruits and carbonated drinks³¹
- Sleep on the left side³²
References :
- Gastroesophageal reflux disease symptoms, diagnosis & treatment. (n.d.). AAAAI | American Academy of Allergy, Asthma & Immunology. https://www.aaaai.org/Conditions-Treatments/Related Conditions/gastroesophageal-reflux-disease fbclid=IwAR0SGKD5UeDfGEg34XuIK6rTQY4PoJqjBaeemjg9ikn2o2U9_2Eq0vT8h3s
- Wu, J. C. (2008). Gastroesophageal reflux disease: An Asian perspective. Journal of Gastroenterology and Hepatology, 23(12), 1785-1793. https://doi.org/10.1111/j.1440-1746.2008.05684.x
- Goh, K. (2011). Gastroesophageal reflux disease in Asia: A historical perspective and present challenges. Journal of Gastroenterology and Hepatology, 26, 2-10. https://doi.org/10.1111/j.1440-1746.2010.06534.x
- Jung, H. (2011). Epidemiology of gastroesophageal reflux disease in Asia: A systematic review. Journal of Neurogastroenterology and Motility, 17(1), 14-27. https://doi.org/10.5056/jnm.2011.17.1.14
- Castell, D. O., & Singh, E. R. (2013). Dysphagia and gastroesophageal reflux disease. Practical Manual of Gastroesophageal Reflux Disease, 239-252. https://doi.org/10.1002/9781118444788.ch14
- Batista, A. O., Nascimento, W. V., Cassiani, R. A., Silva, A. C., Alves, L. M., Alves, D. C., & Dantas, R. O. (2020). Prevalence of non-obstructive dysphagia in patients with heartburn and regurgitation. Clinics, 75, e1556. https://doi.org/10.6061/clinics/2020/e1556
- Upper digestive tract conditions, symptoms and treatment | Gleneagles hospital Singapore. (n.d.). Private Hospital and Medical Center in Singapore | Gleneagles Hospital. https://www.gleneagles.com.sg/facilities-services/centre-excellence/digestive-gut-health/upper-digestive-disorders?gclid=EAIaIQobChMIrZ-ixf2f-AIVyXwrCh3fWg1GEAAYASAAEgJPAfD_BwE
- MacFarlane, B. (2018). Management of gastroesophageal reflux disease in adults: A pharmacist’s perspective. Integrated Pharmacy Research and Practice, 7, 41-52. https://doi.org/10.2147/iprp.s142932
- Song, E. M., Jung, H., & Jung, J. M. (2012). The association between reflux Esophagitis and psychosocial stress. Digestive Diseases and Sciences, 58(2), 471-477. https://doi.org/10.1007/s10620-012-2377-z
- Miller, K. (2008, July 14). Common heartburn triggers. WebMD. https://www.webmd.com/heartburn-gerd/triggers
- Ness-Jensen, E., & Lagergren, J. (2017). Tobacco smoking, alcohol consumption and gastro-oesophageal reflux disease. Best Practice & Research Clinical Gastroenterology, 31(5), 501-508. https://doi.org/10.1016/j.bpg.2017.09.004
- GERD: Can certain medications make it worse? (2020, January 22). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/gerd/expert-answers/heartburn-gerd/faq-20058535
- Fatani, A., Vaher, K., Rivero-Mendoza, D., Alabasi, K., & Dahl, W. J. (2020). Fermented soy supplementation improves indicators of quality of life: a randomized, placebo-controlled, double-blind trial in adults experiencing heartburn. BMC research notes, 13(1), 364. https://doi.org/10.1186/s13104-020-05205-z
- Bogdanov, I. (1979). Gastropharm–a preparation for treatment of gastritis, gastric and duodenal ulcers. Khranitelna promishlenost.
- Hirata, Y. & Uchida, A. (2003) Clinical effects of GASTRO AD for gastritis patients. Japanese Journal of Medicine and Pharmaceutical Science, 49(4), 597-601.
- Wallace, T. D., Bradley, S., Buckley, N. D., & Green-Johnson, J. M. (2003). Interactions of lactic acid bacteria with human intestinal epithelial cells: effects on cytokine production. Journal of food protection, 66(3), 466–472. https://doi.org/10.4315/0362-028x-66.3.466
- Dey, S., Deepak, M., Setty, M., D’Souza, P., Agarwal, A., & Sangli, G. K. (2009). Bioactive caffeic acid esters fromGlycyrrhiza glabra. Natural Product Research, 23(18), 1657-1663. https://doi.org/10.1080/14786410802134348
- Chandrasekaran, C., Deepak, H., Thiyagarajan, P., Kathiresan, S., Sangli, G. K., Deepak, M., & Agarwal, A. (2011). Dual inhibitory effect of Glycyrrhiza glabra (GutGard™) on COX and LOX products. Phytomedicine, 18(4), 278-284. https://doi.org/10.1016/j.phymed.2010.08.001
- Thiyagarajan, P., Chandrasekaran, C. V., Deepak, H. B., & Agarwal, A. (2011). Modulation of lipopolysaccharide-induced pro-inflammatory mediators by an extract of Glycyrrhiza glabra and its phytoconstituents. Inflammopharmacology, 19(4), 235-241. https://doi.org/10.1007/s10787-011-0080-x
- Raveendra, K. R., Jayachandra, Srinivasa, V., Sushma, K. R., Allan, J. J., Goudar, K. S., Shivaprasad, H. N., Venkateshwarlu, K., Geetharani, P., Sushma, G., & Agarwal, A. (2012). An Extract of Glycyrrhiza glabra (GutGard) Alleviates Symptoms of Functional Dyspepsia: A Randomized, Double-Blind, Placebo-Controlled Study. Evidence-based complementary and alternative medicine : eCAM, 2012, 216970. https://doi.org/10.1155/2012/216970
- Schulz, C., Koch, N., Schütte, K., Pieper, D. H., & Malfertheiner, P. (2015). H. pylori and its modulation of gastrointestinal microbiota. Journal of digestive diseases, 16(3), 109–117. https://doi.org/10.1111/1751-2980.12233
- Puram, S., Suh, H. C., Kim, S. U., Bethapudi, B., Joseph, J. A., Agarwal, A., & Kudiganti, V. (2013). Effect of GutGard in the Management of Helicobacter pylori: A Randomized Double Blind Placebo Controlled Study. Evidence-based complementary and alternative medicine : eCAM, 2013, 263805. https://doi.org/10.1155/2013/263805
- Schulz, C., Koch, N., Schütte, K., Pieper, D. H., & Malfertheiner, P. (2015). H. pylori and its modulation of gastrointestinal microbiota. Journal of digestive diseases, 16(3), 109–117. https://doi.org/10.1111/1751-2980.12233
- Puram, S., Suh, H. C., Kim, S. U., Bethapudi, B., Joseph, J. A., Agarwal, A., & Kudiganti, V. (2013). Effect of GutGard in the Management of Helicobacter pylori: A Randomized Double Blind Placebo Controlled Study. Evidence-based complementary and alternative medicine : eCAM, 2013, 263805. https://doi.org/10.1155/2013/263805
- Weinland, S. R., & Drossman, D. A. (2013). Psychological factors and treatments in irritable bowel syndrome. Irritable Bowel Syndrome, 183-213. https://doi.org/10.1002/9781118444689.ch10
26. Yan, F., & Polk, D. B. (2011). Probiotics and immune health. Current opinion in gastroenterology, 27(6), 496–501. https://doi.org/10.1097/MOG.0b013e32834baa4d - Markowiak-Kopeć, P., & Śliżewska, K. (2020). The Effect of Probiotics on the Production of Short-Chain Fatty Acids by Human Intestinal Microbiome. Nutrients, 12(4), 1107. https://doi.org/10.3390/nu12041107
- Didari, T., Mozaffari, S., Nikfar, S. & Abdollahi, M. (2015). Effectiveness of probiotics in irritable bowel syndrome: Updated systematic review with meta-analysis. World Journal of Gastroenterol, 21(10): 3072-3084. https://doi.org/10.3748/wjg.v21.i10.3072
- Vale, F. F., Vítor, J. M., & Oleastro, M. (2016). Probiotics as an alternative therapy for Helicobacter pylori-associated diseases. Helicobacter pylori Research, 543-574. https://doi.org/10.1007/978-4-431-55936-8_24
- Braun L, Cohen M. Herbs and Natural supplements. Ebook 4th edition. Chatswood: Elsevier 2015 pp.771-796.
- Katz, P. O., Dunbar, K. B., Schnoll-Sussman, F. H., Greer, K. B., Yadlapati, R., & Spechler, S. J. (2021). ACG clinical guideline for the diagnosis and management of gastroesophageal reflux disease. American Journal of Gastroenterology, 117(1), 27-56. https://doi.org/10.14309/ajg.0000000000001538
- Person, E., Rife, C., Freeman, J., Clark, A., & Castell, D. O. (2015). A Novel Sleep Positioning Device Reduces Gastroesophageal Reflux: A Randomized Controlled Trial. Journal of clinical gastroenterology, 49(8), 655–659.
You might also be interested in
Brain Fog
- Brain fog is used to describe ‘a usually temporary state of diminished mental capacity marked by inability to concentrate or to think or reason clearly.
- Brain fog is not a formal diagnosis or medical condition but a series of neuropsychologic symptoms related to mild cognitive impairment which may affect daily function.
- Although there are no statistics on the prevalence of brain fog specifically, it was estimated that around 600 million people worldwide suffer from cognitive dysfunction.
- It has been reported that brain fog is one of the most common long COVID symptoms among survivors.³
Constipation
- Constipation is a common functional gastrointestinal disorder, with prevalence in the general population of approximately 20%. It is more prevalent in females and the elderly¹.
- Constipation is both a symptom and, when chronic, a multisymptomatic disorder, and it can overlap with other gastrointestinal tract disorders such as dyspepsia and gastroesophageal reflux disease².
- Constipation most commonly refers to infrequent bowel movements. It is defined as having a bowel movement less than 3 times per week³.
- Chronic constipation is difficult and/or rare passage of stools that lasts for several months that can interfere people’s ability to go about their daily activities. It may also cause people to strain excessively to have bowel movement⁴.




